When you look at treatment options for addiction, the intensive outpatient program therapy structure can seem like a middle ground that is hard to define. You might wonder how it really works day to day, how it differs from inpatient rehab or standard outpatient care, and what makes one IOP more effective than another. Understanding these details helps you decide whether this level of care fits your life and your recovery goals.
Understanding intensive outpatient program therapy structure
An intensive outpatient program, or IOP, provides structured addiction treatment several days per week while you continue living at home. Instead of 24 hour supervision, you attend scheduled therapy blocks, usually in the morning or evening, then return to your normal environment to practice what you are learning.
Many IOPs involve three to five treatment days per week, with sessions that last about three to four hours per day, for a total of 9 to 20 hours weekly, depending on your needs [1]. Programs like those described by Magnolia Medical Group typically ask you to attend four to nine hours of therapy on three to four days each week, focusing on ending substance use while you maintain work and family responsibilities [2].
If you want a deeper overview, you can explore what an intensive outpatient program is in more detail at what is an intensive outpatient program and how intensive outpatient treatment works.
Core elements of an effective IOP
An effective intensive outpatient program therapy structure is more than a set number of hours. The most helpful programs share several core features that work together to support lasting recovery.
Sufficient intensity and frequency
Research based guidelines describe intensive outpatient care as Level II treatment, typically providing 6 to 30 hours of programming across 3 to 5 days each week [3]. This intensity creates enough contact and accountability to disrupt addictive patterns without removing you from your life completely, as inpatient rehab does.
Many effective programs follow structures such as:
- 3 to 5 treatment days each week
- 3 to 4 hours of therapy per treatment day
- At least 9 hours of weekly therapeutic services, which is also the minimum for Medicare coverage of IOP services [4]
You can see typical time commitments and weekly loads at how many hours is an intensive outpatient program.
Individualized treatment planning
While you share groups with peers, your treatment plan should be your own. Effective IOPs complete a thorough assessment first, then build a plan that accounts for:
- Substance use history and severity
- Co occurring mental health conditions like anxiety, depression, or trauma
- Family situation and support network
- Work, school, and caregiving responsibilities
- Legal or financial stressors
Programs such as Magnolia Medical Group emphasize that therapists monitor your progress and adjust sessions and supports as needed, rather than following a rigid script [2].
This individualized approach is especially important if you live with co occurring mental health symptoms, something OhioGuidestone specifically targets through counseling that addresses anxiety, depression, and loneliness alongside substance use [5].
Mix of evidence based therapies
You benefit most when your intensive outpatient program uses methods that are supported by research. Effective IOPs draw from several modalities, often including:
- Cognitive behavioral therapy to help you identify and change thought patterns and behaviors that support substance use
- Motivational approaches to strengthen your internal reasons for change
- 12 step facilitation or similar mutual help frameworks to connect you with ongoing community support
- Psychoeducational groups that build understanding of addiction, relapse, and coping skills
- Community reinforcement or contingency management models that reward healthy behavior [6]
Some programs, such as Penn Medicine’s IOP, combine CBT, motivational interviewing, creative arts therapies, and psychoeducational groups to tailor care to each person’s needs [7].
You can learn more about how these approaches support change at how intensive outpatient therapy helps addiction.
Combination of group, individual, and family work
The structure of your therapy sessions matters just as much as the number of hours. Effective IOPs typically include:
- Group therapy as the primary setting for skill building, support, and accountability
- Individual therapy for deeper one on one work around trauma, mental health, or personal barriers
- Family or couples sessions to repair relationships and strengthen your support system
Providence Treatment describes IOPs that blend individual therapy, group sessions, and educational components to address the emotional, psychological, and social aspects of recovery [8].
Penn Medicine also integrates group, individual, psycho educational, and family sessions within its substance use IOP [7].
Typical schedules in intensive outpatient programs
Understanding what your week might look like in an IOP can help you picture how it fits into your life.
Weekly time commitment
Across different providers, you commonly see:
- 3 to 5 days per week in treatment
- 3 to 4 hours of programming per treatment day
- A total of 8 to 20 hours per week, depending on your clinical needs and program design [9]
Some programs, such as OhioGuidestone, require at least 10 hours per week and typically last 8 to 12 weeks [5]. Others, like Penn Medicine, may provide intensive care for several months followed by less intensive outpatient services for up to a year, with frequency stepping down as you stabilize [7].
To see how this might translate to your calendar, you can read more at intensive outpatient program schedule for addiction.
Daytime, evening, and telehealth options
Flexibility is one of the main advantages of IOP. Many programs offer:
- Morning tracks for people who work evenings or nights
- Evening tracks for those with daytime jobs or caregiving roles
- Telehealth or hybrid options so you can attend virtually when appropriate
OhioGuidestone, for example, provides both in person and telehealth sessions with day and evening options to help you maintain family and job commitments [5].
If you are trying to maintain employment while in treatment, it can help to review can you work while in an intensive outpatient program.
How long an effective IOP usually lasts
You may also be asking how long you will need this more intensive structure before you can step down.
Common program lengths
Different organizations describe IOP durations in a similar range:
- 4 to 6 weeks for some shorter, focused programs [6]
- 8 to 12 weeks as a common standard [10]
- 90 days or longer when possible, since treatments of at least three months are often associated with better outcomes in substance use disorder recovery [3]
Providence Treatment notes that extended IOPs may last 12 weeks or more for people with complex needs such as severe addiction or significant co occurring mental health disorders [8].
Some programs, including Penn Medicine, may involve about 3 or more months of intensive outpatient treatment followed by 6 to 9 months of less intensive outpatient services, depending on your progress and needs [7].
For a closer look at time frames and phases, see how long does an iop program last.
Staged and stepdown structure
Effective IOPs usually follow stages rather than a single uniform block of care. The NCBI guidelines describe two core early stages:
- Stage 1, treatment engagement, focuses on building commitment, stabilizing crises, and establishing a working treatment contract
- Stage 2, early recovery, emphasizes education, group involvement, and developing skills for a substance free lifestyle [3]
As you progress, you often step down to fewer hours per week or transition to Level I outpatient care, such as weekly sessions. Planned stepdown care and an individual transition plan support continuity and reduce the risk of dropping out [3].
Understanding these stages can help you anticipate the steps in an intensive outpatient program and how your care may change over time.
A useful way to think about an effective IOP is as a bridge: intensive enough to stabilize you and build new habits, yet designed to connect you back to everyday life and ongoing community support.
Comparing IOP with inpatient and standard outpatient care
To decide whether intensive outpatient is the right level of care, it helps to compare it directly with other options.
IOP vs inpatient rehab
Inpatient rehab requires you to live at the facility with 24 hour supervision, usually for 30 to 90 days or longer. This level of care is often recommended if you:
- Have severe physical dependence or need medical detox
- Face high risk withdrawal or serious medical complications
- Live in an unsafe or highly triggering environment
- Have repeatedly relapsed after lower levels of care
IOP, by contrast, treats you several days per week while you sleep at home. It allows you to keep more independence and stay engaged with work or family while still receiving intensive therapy.
You can explore this comparison further at iop vs inpatient rehab and when to choose intensive outpatient rehab.
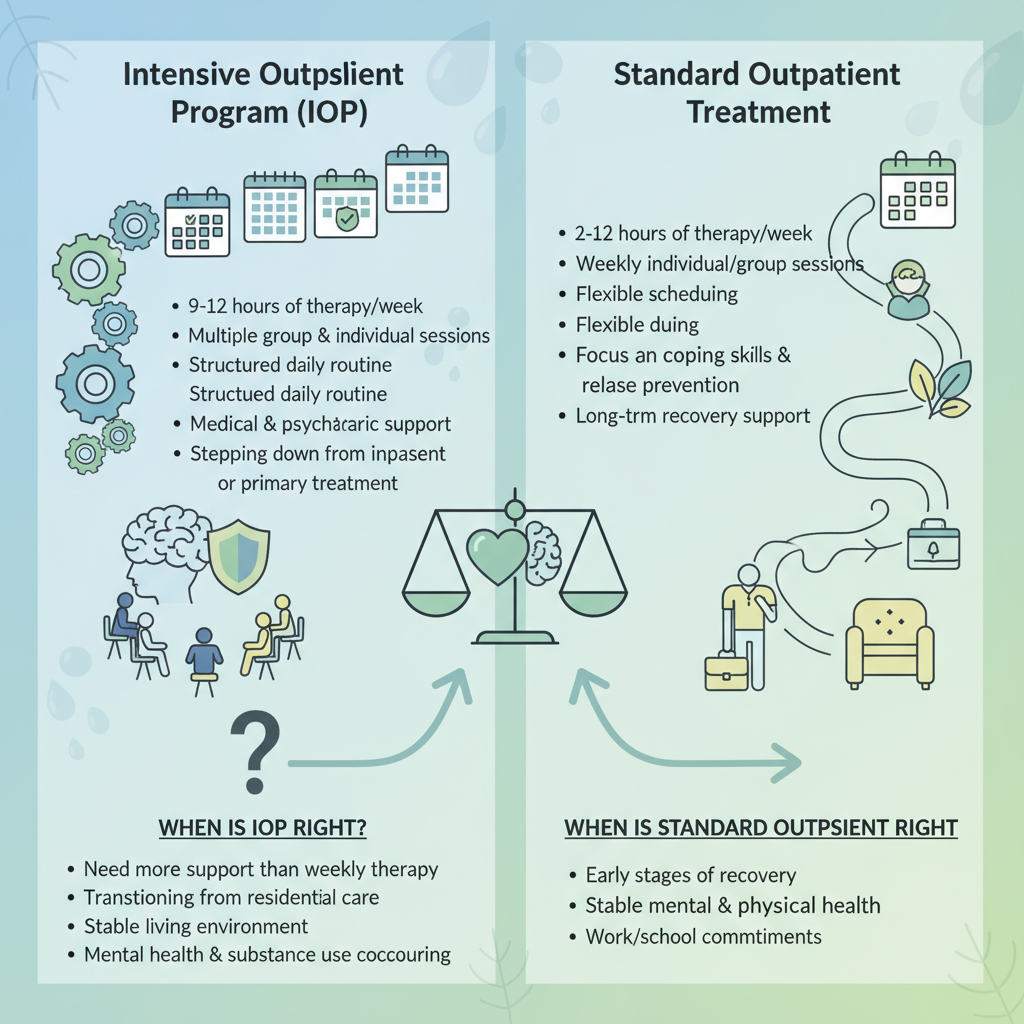
IOP vs traditional outpatient addiction treatment
Standard outpatient care usually involves one individual therapy session per week or occasional group sessions. This lower intensity may be enough for:
- Mild substance use disorders
- People who have already completed higher levels of care and are in stable recovery
- Those who primarily need maintenance and support rather than intensive change work
IOPs provide a middle ground between weekly therapy and full residential treatment. You typically participate in 3 to 5 sessions per week, which creates more structure, accountability, and skill practice opportunities than traditional outpatient care offers [6].
You can compare more details at iop vs outpatient addiction treatment.
Who an intensive outpatient therapy structure is best for
Not everyone needs or benefits from the same level of care. An IOP structure tends to fit best if you:
- Need more than weekly therapy but do not require 24 hour supervision
- Have a relatively stable living environment that is not actively unsafe or dominated by substance use
- Can manage basic daily responsibilities with support
- Are medically and psychiatrically stable enough to be treated in an outpatient setting
- Are willing to attend multiple sessions each week and participate actively
Programs like Mirmont’s IOP for mental health serve people who need more support than once weekly therapy but do not require inpatient care, including adolescents, young adults, and those with co occurring mental health and substance use concerns [11].
Medicare’s criteria for IOP coverage also provide a useful benchmark. To qualify, your care plan must show you need at least 9 hours of therapeutic services per week for a mental health or substance use condition, even though you do not require inpatient hospitalization [4].
For more help deciding if this fits your situation, you can read who qualifies for intensive outpatient treatment, who should attend an intensive outpatient program, and when to choose intensive outpatient rehab.
What makes an IOP structure effective in practice
When you look beyond schedules and session counts, certain practical qualities tend to make an intensive outpatient program therapy structure more effective for real world recovery.
Integration with everyday life
IOPs are uniquely positioned to let you test skills in real time. Because you go home after sessions, you can:
- Practice coping strategies at work, school, and in family settings
- Bring back real experiences, setbacks, and successes to process in therapy
- Adjust your plan quickly as new challenges appear
Magnolia Medical Group notes that this structure lets you apply what you learn immediately to work and family situations, supporting long term sobriety without requiring full hospitalization [2].
This real life integration is one of the main benefits of intensive outpatient treatment and a key reason many people choose it.
Supportive community and peer involvement
Group therapy and peer support are central to most IOPs. Effective structures create:
- A consistent group of peers who attend together
- Space to share experiences, setbacks, and victories
- Built in accountability to show up and stay engaged
Group therapy sessions in IOPs foster a sense of belonging, accountability, and hope, which can be crucial for sustained recovery [8].
Some programs also include certified peer recovery specialists who draw on their own lived experience to provide one on one support. OhioGuidestone’s IOP uses peer specialists certified by the state of Ohio to enhance engagement and outcomes [5].
If you want to understand how this social structure helps you change, you can review how iop helps addiction recovery.
Wrap around and practical support
Addiction rarely exists in isolation. Effective IOPs recognize that you may also be dealing with:
- Strained or broken family relationships
- Housing instability
- Employment and financial challenges
- Legal issues
OhioGuidestone’s IOP, for example, incorporates wrap around services to help clients address these related life challenges, not only the addiction itself [5].
This broader support reduces stressors that might otherwise push you back toward substance use and strengthens the foundation for long term change.
Medication and adjunctive therapies when needed
If you take psychiatric medications or benefit from medication assisted treatment for opioid or alcohol use disorder, a strong IOP structure will:
- Offer psychiatric assessment and medication management
- Coordinate with prescribers and primary care
- Integrate medication decisions with your therapy goals
Verywell Mind notes that IOPs often include medication management by psychiatrists alongside traditional therapy [6]. Some programs also incorporate adjunctive therapies like EMDR, TMS, equine therapy, or yoga to complement psychotherapy when appropriate [6].
Medicare Part B explicitly covers IOP services for mental health and substance use disorders, including those delivered in opioid treatment programs for opioid use disorder, as long as the program meets certain criteria [4].
What to expect when you start an IOP
If you decide to enroll, knowing what the first weeks look like can reduce anxiety and help you prepare.
You can typically expect:
- Intake and assessment where clinicians gather your history, current symptoms, and goals
- Creation of a personalized treatment plan that outlines your schedule, therapy types, and specific objectives
- Orientation to group norms including confidentiality, attendance expectations, and safety guidelines
- Early engagement work which may focus on stabilizing crises, building motivation, and establishing a safety plan
- Regular progress reviews to track changes, adjust your plan, and discuss readiness to step down
Programs such as Penn Medicine schedule intensive group sessions several days per week and require an intake assessment before enrollment so that services can be matched to your needs [7].
To walk through these stages in more depth, you can visit what to expect in an iop program, iop program requirements, and addiction recovery intensive outpatient structure.
Deciding whether an IOP structure is right for you
When you put all of this information together, an intensive outpatient program therapy structure may be a good fit if:
- You need more structured support than once weekly therapy provides
- You want to remain at home and keep working or caring for family
- Your home environment is generally safe and not dominated by active substance use
- You are medically stable enough for outpatient care
- You are ready to commit to multiple therapy sessions each week
If you still feel unsure, it can help to talk with a treatment professional who can assess your situation and suggest the appropriate level of care. You can also explore how effective are intensive outpatient programs to see how this level of treatment performs over time.
Understanding how intensive outpatient treatment works, how it compares with other options, and what makes its therapy structure effective gives you a stronger foundation to choose the care that matches where you are in your recovery journey.