Understanding what an intensive outpatient program is
If you are trying to decide what level of addiction treatment you need, one of the most common questions is, “what is an intensive outpatient program, and how does it fit between inpatient rehab and weekly therapy?”
An Intensive Outpatient Program, often called an IOP, is a structured form of addiction and mental health treatment that provides several hours of therapy on multiple days each week, while you continue living at home. Sessions usually run two to three hours a day, three to five days a week, which is significantly more support than traditional outpatient therapy that might involve one session a week [1].
In the American Society of Addiction Medicine (ASAM) system, IOP is considered a Level II service. It offers more structure than standard outpatient care (Level I) and less than residential or inpatient treatment (Level III) [2]. For substance use disorders, an IOP typically provides at least 9 to 12 hours of structured therapy activities each week, often in three 3 hour sessions, while you remain in your home environment [3].
If you want a deeper dive into how the model works in practice, you can review how intensive outpatient treatment works in more detail at how intensive outpatient treatment works.
How intensive outpatient treatment works
In an IOP, you typically participate in a mix of group therapy, individual counseling, psychoeducation, and sometimes family sessions. The exact structure can vary from program to program, but several core elements are common across most reputable IOPs.
Typical components include:
- Group therapy focused on relapse prevention, coping skills, and peer support
- Individual therapy that targets your specific challenges and goals
- Psychoeducational groups that teach you about addiction, mental health, and recovery
- Medication management or psychiatry visits if you have co-occurring mental health conditions
- Skills based groups that may include mindfulness, stress management, communication, or life skills
Many programs draw on therapies that have been studied extensively. Common modalities in IOPs include 12 Step facilitation, Cognitive Behavioral Therapy (CBT), motivational approaches, therapeutic community models, the Matrix Model, and contingency management that uses rewards to reinforce positive behaviors [4].
Because you remain in your day to day environment, IOP is designed to give you tools that you immediately practice in real life. This is one of the reasons research has found that intensive outpatient treatment can be as effective as inpatient or residential treatment for many people, with similar outcomes in reducing substance use and supporting abstinence across diverse patient groups [2].
To see more about how sessions are structured, visit intensive outpatient program therapy structure or steps in an intensive outpatient program.
Typical schedule and time commitment
When you ask, “what is an intensive outpatient program,” you are often also asking how it will fit into your daily life. Time commitment is a key factor.
Most IOPs require at least 9 to 12 hours per week of treatment activities. This is usually scheduled as three or four days a week, with each session lasting around three hours [3]. Some programs, like the Meadows Intensive Outpatient Program, provide three hours of group therapy four days per week, plus one individual therapy session and a weekly psychiatry session [5].
A typical IOP day might look like this:
- Check in and brief mindfulness or grounding
- Therapist led group therapy focused on a specific topic such as triggers, cravings, or communication
- Short break
- Psychoeducational or skills group on topics like relapse prevention, coping skills, or mental health education
- Closing check out and setting intentions or goals for the time between sessions
Many programs offer morning, evening, or weekend groups to accommodate work or family responsibilities. For example, some IOPs run Monday, Wednesday, and Friday from 9:00 am to 12:30 pm, with additional evening and Saturday options [6].
If you want to see how this can look over a full week, you can explore an intensive outpatient program schedule for addiction as a reference. For more detail on hours and timeframes, visit how many hours is an intensive outpatient program.
How long an IOP usually lasts
Length of stay in an intensive outpatient program can vary based on your needs, progress, and the specific model of the program.
Many IOPs designed for mental health or addiction treatment last about four to six weeks, with multiple sessions per week [1]. Some substance use programs extend longer, especially when they are part of a full continuum of care.
For example, the IOP at Penn Medicine often lasts up to one year in total. It may begin with three or more months of intensive outpatient treatment, followed by six to nine months of step down outpatient services, with the exact length adjusted based on your progress and needs [6].
Duration is usually individualized and may change over time. If you stabilize quickly, you may move to less intensive care sooner. If you need more support, your team might recommend extending your IOP or shifting to a higher level of care.
For a closer look at timing and phases, you can read more at how long does an iop program last.
Who an intensive outpatient program is best for
Not everyone is a good fit for IOP. Understanding who typically benefits most can help you decide whether this level of care is right for you.
In general, an IOP is well suited for you if:
- You have a substance use disorder or co occurring substance and mental health condition
- You do not need 24 hour medical supervision or medically managed detoxification
- Your condition is stable enough that you can remain safe at home
- You are motivated to participate in treatment several times a week
- You can maintain basic daily functioning with support, such as living in a stable environment or having some level of social support
Intensive outpatient programs were originally developed in the 1980s to help working professionals access treatment without leaving their jobs, and over time they have expanded to serve a wide range of people. By 2019, roughly 16,000 facilities were providing IOP services to about 1.4 million clients [1].
Many people enter IOP for one of two main reasons. Either they need more help than weekly outpatient therapy because there is a concern about relapse or hospitalization risk, or they are stepping down from inpatient or residential care and need support transitioning back to daily life [1].
To explore fit in more depth, you can review who qualifies for intensive outpatient treatment and who should attend an intensive outpatient program.
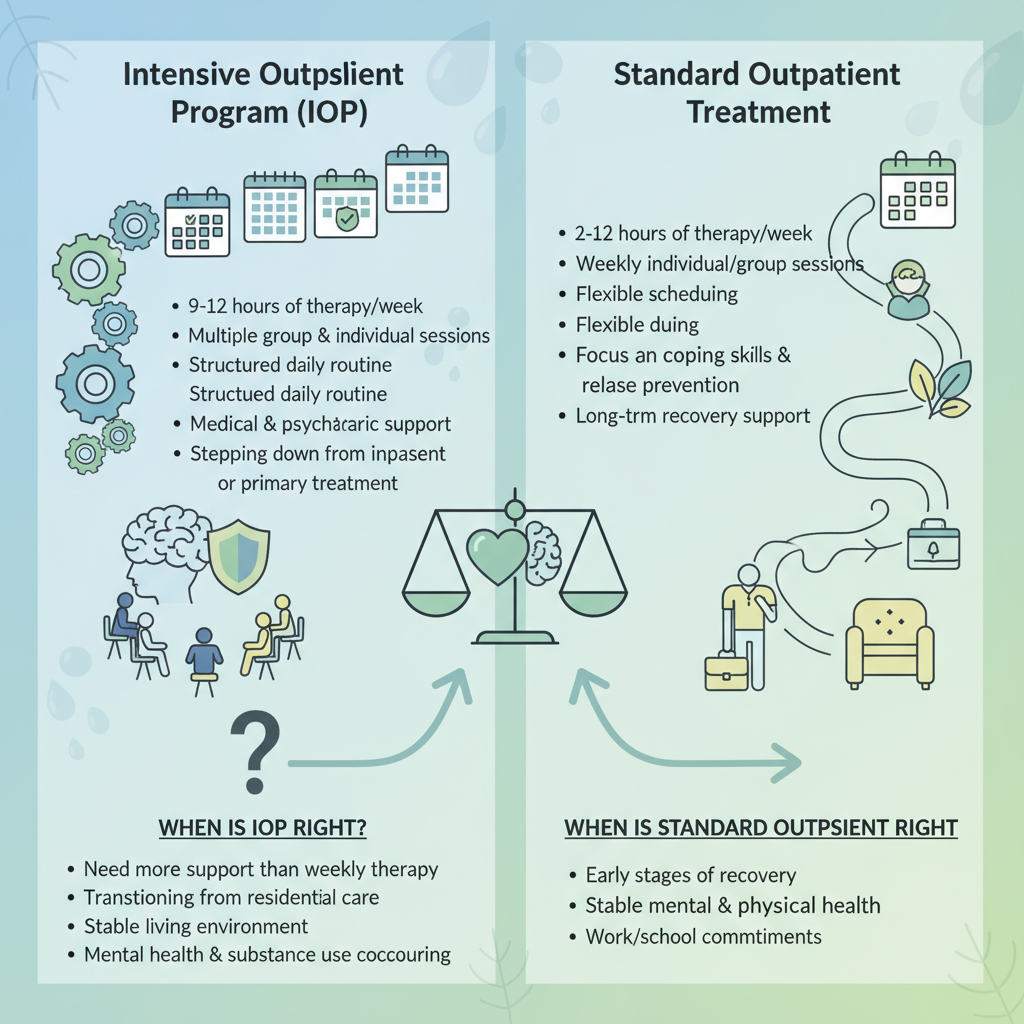
Comparing IOP, inpatient, and standard outpatient care
When you try to decide if IOP is the right level of care, it helps to see where it sits compared to other options.
| Level of care | Living situation | Typical time in treatment per week | Best suited for |
|---|---|---|---|
| Standard outpatient | Live at home | Usually 1 to 4 hours weekly [5] | Mild to moderate symptoms, strong support, lower risk of relapse or harm |
| Intensive outpatient program (IOP) | Live at home | At least 9 to 12 hours weekly, often 3 to 4 days a week [3] | Moderate symptoms, need for more structure than weekly therapy, but not needing 24 hour care |
| Inpatient or residential rehab | Live onsite in a facility | 24 hour care, full day schedules | Severe symptoms, medical detox needs, lack of safe home environment, high risk of harm or relapse without supervision |
IOP offers a middle path. It is more intensive and structured than traditional outpatient therapy, which might only provide 4 to 10 hours of treatment per week, yet it allows you to stay at home and maintain some daily routines. This can be an advantage if you want to keep working, attending school, or caring for family, while still receiving a high level of support [7].
For a deeper comparison, you may find it helpful to review iop vs inpatient rehab and iop vs outpatient addiction treatment.
Benefits of choosing an intensive outpatient program
If you are trying to decide whether an IOP is the right choice, it helps to understand the specific benefits this level of care can offer. Research has found that intensive outpatient programs are as effective as inpatient or residential treatment for many individuals in reducing substance use and supporting abstinence [2].
Key benefits often include:
- A higher level of structure than standard outpatient therapy, without requiring you to live onsite
- The ability to remain in your home and community, where you can immediately practice new coping and relapse prevention skills in real life situations [2]
- Flexible, part time care that lets you keep working, going to school, or managing responsibilities when clinically appropriate [8]
- A continuous connection with therapists and peers, which can reduce the sense of isolation and increase accountability
- Opportunities to involve family or significant others in treatment if that is supportive for you
Because IOPs use evidence based approaches such as CBT, motivational interviewing, and 12 Step facilitation, they focus not only on abstinence but also on building long term skills and resilience [9]. The goal is to help you navigate triggers, manage mental health symptoms, and sustain recovery over time [8].
If you want a more detailed breakdown of advantages, you can explore the benefits of intensive outpatient treatment and how IOP specifically supports change at how iop helps addiction recovery.
What to expect day to day in an IOP
Knowing what your daily experience will look like can make the choice feel less overwhelming. While each program is unique, you can generally expect a structured routine and a mix of therapeutic activities.
Common elements of an IOP day include:
- Opening check in to assess your mood, cravings, and any safety concerns
- Group sessions using CBT, relapse prevention, or motivational approaches to help you recognize triggers, change unhelpful thought patterns, and build healthier coping strategies [9]
- Psychoeducation about addiction, mental health conditions, medications, and wellness
- Skills practice, such as role plays, communication exercises, or mindfulness
- Occasional family or couples sessions, if appropriate and part of your treatment plan
- Closing check out, including goal setting and planning how you will use your skills between sessions
Some IOPs also incorporate expressive arts therapies, yoga, or other holistic activities alongside core evidence based counseling, to support your physical and emotional well being [10].
For more detail on what the process feels like, you can review what to expect in an iop program and addiction recovery intensive outpatient structure.
Balancing IOP with work, family, and daily life
A common concern is whether you can realistically participate in an IOP while managing your responsibilities. Because intensive outpatient programs are designed as part time treatment, many people are able to continue working, studying, or caring for family while in care.
IOP typically involves fewer hours than a Partial Hospitalization Program (PHP), which often runs closer to a full day schedule, yet more hours than weekly outpatient counseling. This flexible structure is meant to support recovery without completely disrupting your daily routine [8].
Evening or early morning groups can make it easier to attend without missing work. Some employers will work with you to adjust hours temporarily, especially if you explain that you are receiving treatment.
If you are wondering how employment fits specifically, you can learn more at can you work while in an intensive outpatient program.
When an IOP may not be the right choice
Even though IOP is appropriate for many people, there are times when another level of care is safer or more effective. You might need inpatient, residential, or medical detox instead of IOP if:
- You require 24 hour medical supervision, for example during alcohol or benzodiazepine withdrawal
- You have recently made a serious suicide attempt or have active plans to harm yourself or others
- Your home environment is unsafe, unstable, or strongly associated with ongoing substance use
- You have tried IOP or outpatient treatment several times without improvement, and your team believes you need more intensive support
- You are unable to attend sessions consistently because of transportation, housing, or legal issues
In these cases, a higher level of care can help stabilize you before you transition to IOP. On the other end of the spectrum, if your symptoms are relatively mild and you are functioning well at work and home, traditional outpatient therapy may be an appropriate starting point.
You can explore these decision points further at when to choose intensive outpatient rehab and how intensive outpatient therapy helps addiction.
How to decide if an IOP is the right next step
Ultimately, deciding if an intensive outpatient program is right for you is a collaborative process. It usually involves a professional assessment, your personal goals, and an honest look at your current level of risk and support.
You are more likely to benefit from IOP if you:
- Feel that weekly therapy alone is not enough structure or accountability
- Want to avoid or step down from inpatient care but still need frequent contact with a treatment team
- Have a relatively safe and stable place to live while you work on recovery
- Are ready to commit to attending sessions multiple times per week and doing work between them
A comprehensive evaluation will often include a review of your substance use history, mental health symptoms, medical conditions, past treatment attempts, social support, and daily functioning. Based on this information, your clinician can help you choose between standard outpatient care, IOP, PHP, or inpatient treatment.
If you want to understand the effectiveness of this choice, you can look at outcomes discussed in how effective are intensive outpatient programs. For a more decision focused overview, when to choose intensive outpatient rehab can help you weigh your options.
You do not need to make this decision alone. Reaching out for an assessment is often the first step in finding the level of care that matches what you need right now, with the flexibility to adjust as you grow in recovery.