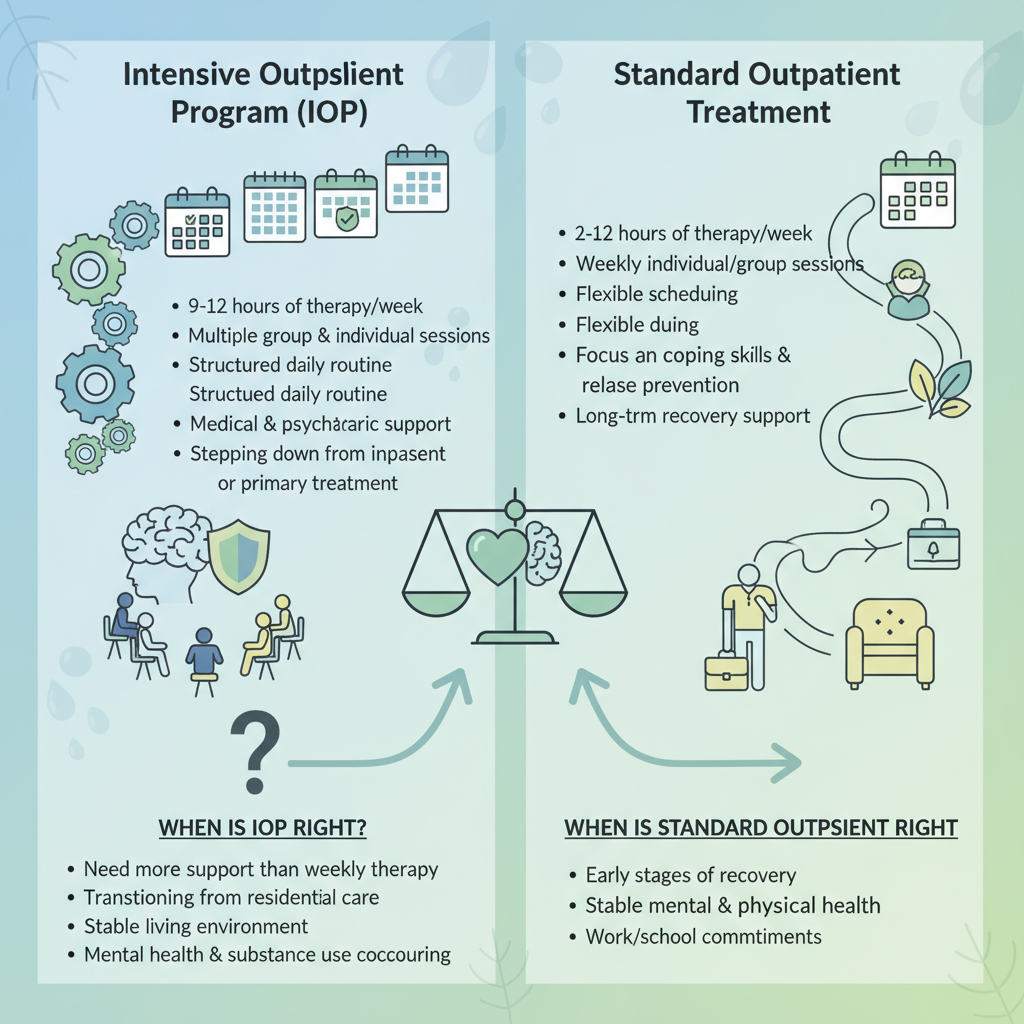
Understanding how intensive outpatient treatment works
If you are comparing levels of care, understanding how intensive outpatient treatment works can help you decide what kind of structure you need to stay sober. Intensive outpatient programs, often called IOPs, sit between weekly outpatient therapy and 24/7 inpatient rehab. They give you several hours of focused treatment each week while you continue living at home.
In an IOP, you typically attend treatment multiple days per week for 2 to 4 hours at a time. Programs use evidence-based therapies, education, and peer support to help you build relapse prevention skills, stabilize your mental health, and practice recovery tools in your daily life. Many adults choose IOP because it provides a high level of support without completely stepping away from work, school, or family.
To see where IOP fits in the broader picture of care, you can also explore what an intensive outpatient program is in more detail at what is an intensive outpatient program.
Where intensive outpatient fits in the levels of care
You might be deciding between inpatient rehab, standard outpatient counseling, and IOP. Each level of care offers a different amount of structure, time in treatment, and supervision.
An intensive outpatient program is considered a mid-level or “step up / step down” level of care. It is more structured than weekly outpatient therapy but less restrictive than residential or inpatient treatment.
A simple comparison looks like this:
| Level of care | Typical weekly treatment hours | Living situation | Main purpose |
|---|---|---|---|
| Standard outpatient | 1 to 3 hours | You live at home | Ongoing support, early intervention |
| Intensive outpatient (IOP) | 9 or more hours for adults | You live at home or in sober housing | Structured treatment and relapse prevention without 24/7 care |
| Partial hospitalization (PHP) | About 20 or more hours | You live at home or in sober housing | Daytime hospital-level care without overnight stay |
| Inpatient / residential | 24/7 care | You live at the facility | Medical stabilization, detox, high-risk situations |
Research suggests that IOPs usually involve at least 9 treatment hours per week for adults, often spread across 3 to 5 days of programming [1]. Other sources describe IOP as providing at least 6 hours weekly for adolescents and 9 hours weekly for adults, usually delivered over 3 to 5 days per week [2].
If you want a deeper comparison between IOP and other options, you can read more at iop vs inpatient rehab and iop vs outpatient addiction treatment.
What happens in intensive outpatient treatment
Although every program is slightly different, most IOPs follow a similar structure. When you enter an IOP, you will complete an assessment, then your treatment team creates a personalized plan based on your substance use history, mental health, home situation, and goals.
Across different programs, intensive outpatient treatment commonly includes:
- Group therapy sessions
- Individual counseling
- Psychoeducation about addiction and mental health
- Skills training and relapse prevention
- Family therapy or family education
- Medication management or psychiatric care where needed
Evidence-based therapies like cognitive behavioral therapy, motivational interviewing, medication-assisted treatment, and 12 Step facilitation are widely used in IOPs [3]. Some programs also integrate holistic and complementary therapies such as yoga, mindfulness, or expressive arts to support emotional regulation and overall wellness [4].
To see how these services are usually organized day to day, you can explore an example intensive outpatient program schedule for addiction and a more detailed look at intensive outpatient program therapy structure.
Typical IOP schedules and time commitment
One of the most common questions you may have is how many hours an IOP actually takes. While there is some variation, several guidelines are consistent across reputable programs.
Research and major organizations describe IOP schedules in a similar way:
- At least 9 treatment hours per week for adults, usually across 3 or more days [5]
- Often structured as three 3-hour sessions, such as Monday, Wednesday, and Friday [3]
- Some programs run 4 days per week with 3 hours per day of group therapy plus individual and psychiatry sessions [6]
- Others offer morning, afternoon, or evening tracks to fit work and family schedules [7]
Many IOPs also follow a recommendation of at least 90 days of care to support better outcomes, though your exact length of stay will be based on your clinical needs, supports, and progress [1]. More broadly, IOPs often last between 4 and 12 weeks, with some extended programs continuing for 6 months or longer if needed [3].
You can get more detailed answers to scheduling questions at how many hours is an intensive outpatient program, how long does an iop program last, and addiction recovery intensive outpatient structure.
Stages and steps in an IOP program
To understand how intensive outpatient treatment works over time, it helps to look at the stages you typically move through. Many IOPs build on a two-stage model described in treatment research.
Stage 1: Engagement and stabilization
In the first phase, your treatment team focuses on getting you engaged and helping you stabilize. This usually includes:
- Building a working relationship with your therapist and group
- Creating a safety plan and crisis plan
- Addressing any immediate risks or crises
- Beginning to track cravings, triggers, and high-risk situations
This engagement stage is designed to help you stay in treatment long enough to benefit from it and to stabilize any acute concerns [1].
Stage 2: Early recovery and skill building
Once you are more stable and engaged, the program shifts into a more structured early recovery phase. This stage typically involves:
- Educational sessions about addiction, brain changes, and recovery
- Relapse prevention training and coping skills practice
- Ongoing group therapy and individual counseling
- Work on emotional regulation, communication, and relationship issues
Research on integrated IOPs that combine psychoeducation, mindfulness, emotional regulation, and group support has found high satisfaction and strong engagement, with clients reporting average experience ratings above 9 out of 10 [8].
Most programs will walk you through each step in a clear, structured way. If you want to see this broken down in more detail, you can explore steps in an intensive outpatient program and what to expect in an iop program.
Types of therapy and services you receive
The heart of IOP is the mix of therapies and services that support your recovery. While programs vary, you can expect a combination that usually looks like this:
Group therapy and psychoeducation
Group sessions make up a large part of most IOP schedules. These groups give you a chance to:
- Share experiences with people who understand what you are going through
- Practice new coping skills in a supportive setting
- Learn about addiction, mental health, relapse warning signs, and healthy communication
Education and group involvement are core components of the early recovery stage in intensive outpatient treatment [1].
Individual therapy and psychiatric care
In addition to groups, you will typically meet one-on-one with a therapist on a regular basis, often weekly. Some programs also include:
- Psychiatric assessments and medication management
- Regular check-ins about your progress and goals
- Case management support to connect you with housing, medical care, or community resources
For example, some IOP models include weekly individual therapy and weekly psychiatry sessions alongside group work [9].
Family involvement and holistic supports
Many IOPs include family education or therapy so that your loved ones can understand addiction, learn how to support your recovery, and address relationship patterns that might affect your progress [3].
Some programs integrate holistic or complementary therapies such as:
- Mindfulness and meditation
- Yoga and movement-based practices
- Expressive arts
- Acupuncture for sleep, anxiety, or pain relief
Integrated programs that combine evidence-based therapies, complementary methods, and a strong focus on relationships and emotional support often show promising results for people with both substance use and mental health conditions [8].
To see how these elements come together in practice, you can read more at how intensive outpatient therapy helps addiction and how iop helps addiction recovery.
Who intensive outpatient treatment is best for
Intensive outpatient treatment is not the right fit for everyone. It works best for certain situations and needs.
According to national guidelines and leading providers, IOP is particularly appropriate if you:
- Have already completed medical detox, or do not need detox
- Are medically and psychiatrically stable enough to be safe without 24/7 supervision
- Have manageable mental health symptoms and a relatively low risk of severe withdrawal
- Have a safe, substance-free home or can live in sober housing
- Have transportation to get to and from the program
- Are motivated to work on recovery and can participate in group therapy [10]
IOP can serve as:
- An entry point to treatment after detox
- A step-down from inpatient or residential rehab
- A step-up from standard outpatient therapy when you need more structure [11]
If you are unsure whether you meet the clinical and practical requirements for this level of care, you can review who qualifies for intensive outpatient treatment, who should attend an intensive outpatient program, and iop program requirements.
How IOP compares to inpatient and standard outpatient care
When you are deciding how intensive outpatient treatment fits your needs, it helps to think through how it compares with the other main levels of care.
Compared to inpatient rehab
Inpatient or residential treatment provides 24/7 supervision and a fully structured environment. This level of care is often recommended if you:
- Need medical detox or have high medical risk
- Are at high risk of relapse or harm to yourself
- Do not currently have a safe, stable, or substance-free living situation
IOP does not provide overnight supervision or medical detox, but it does give you frequent contact with clinicians, peers, and support. Many people transition from inpatient rehab to IOP as a way to step down in intensity while still having strong therapeutic support [6].
You can look more closely at this comparison at iop vs inpatient rehab.
Compared to standard outpatient treatment
Standard outpatient therapy usually involves weekly or biweekly individual sessions. This can be helpful for maintenance or mild substance use concerns but may not be enough if you:
- Have a more severe addiction
- Are early in recovery and facing frequent triggers
- Have multiple relapses despite seeing a therapist
- Need more structure and accountability
IOP provides several hours of treatment weekly, more frequent touch points, and more support from peers and clinicians than typical outpatient counseling [12].
For a direct comparison, you can explore iop vs outpatient addiction treatment.
Practical considerations: Work, cost, and logistics
Deciding whether IOP fits your life also means thinking through practical issues like work, insurance, and family responsibilities.
Balancing IOP with work or school
One of the main advantages of IOP is that you return home at the end of each day and can often continue with work or school. Many programs offer:
- Morning groups before work
- Afternoon sessions
- Evening or virtual options to reduce disruption to your schedule [13]
Virtual IOP models have also expanded access, particularly for teens and young adults, by letting you attend multiple sessions per week from home with individual, group, and family therapy plus medication management as needed [14].
If you are wondering how employment fits with treatment, you can read more at can you work while in an intensive outpatient program.
Insurance coverage and costs
Medicare Part B describes IOP as a covered mental health service for conditions such as substance use disorders. Coverage usually applies when your treatment plan calls for at least 9 hours of therapeutic services per week, and services can be delivered in hospitals, community mental health centers, Federally Qualified Health Centers, and Rural Health Clinics [15].
For Opioid Use Disorder, IOP services are covered when provided by certified opioid treatment programs. Under Medicare Part B, you generally pay 20 percent of the approved amount after meeting your deductible, although your final costs depend on the type of facility, whether the provider accepts assignment, and any additional insurance you may have [15].
Private insurance plans often follow similar criteria and may cover IOP when it is medically necessary. It is always a good idea to verify your benefits directly with your insurer or the program you are considering.
Why intensive outpatient treatment matters for your recovery
Understanding how intensive outpatient treatment works can help you decide whether this level of care is the right step for you. IOP matters because it offers:
- Enough structure and intensity to support real change
- Flexibility to stay connected to your family, work, or school
- A bridge between higher and lower levels of care so you do not have to leap from inpatient to weekly therapy or vice versa
Several key benefits stand out:
- Strong relapse prevention focus for people who do not need 24/7 supervision [3]
- More treatment hours and support than standard outpatient therapy, while still allowing you to live at home [2]
- High satisfaction and positive experiences in integrated programs that combine education, skills training, emotional support, and holistic practices [8]
If you want to explore the advantages in more depth, you can read about the benefits of intensive outpatient treatment and how effective this level of care can be at how effective are intensive outpatient programs.
You might still be deciding whether to move into IOP now, stay in outpatient care, or consider inpatient. A helpful next step is to look at when to choose intensive outpatient rehab. You can also return to the overview at addiction recovery intensive outpatient structure as you think through what kind of support you need for the next phase of your recovery.
References
- (NCBI Bookshelf)
- (NAMI)
- (American Addiction Centers)
- (Meadows Outpatient, NCBI PMC)
- (NCBI Bookshelf, NAMI)
- (Meadows Outpatient)
- (UPMC)
- (NCBI PMC)
- (Meadows Outpatient, UPMC)
- (American Addiction Centers, NAMI)
- (American Addiction Centers, Meadows Outpatient)
- (Meadows Outpatient, NAMI)
- (UPMC, Charlie Health)
- (Charlie Health)
- (Medicare.gov)